|
During surgery, electrical energy can be applied to tissues to produce a wide variety of effects. Modern electrosurgical devices allow the surgeon to vary the type of waveform that is selected, the power (wattage) that is applied, and the size and shape of the operating element (electrode) that is used.
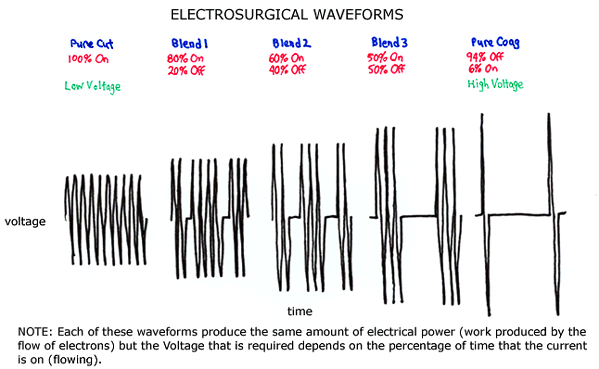
Pure cutting current (volume of electron flow per second) delivers a continuous high frequency flow of electrons to the tissue. Activation of the electrode immediately prior to touching the target tissue produces a plume (of vapor) between the electrode and the tissue, such that the current cuts through the tissue by vaporizing (exploding) the cells without significantly elevating the tissue temperature. Therefore, lateral thermal damage (burn injury) to surrounding tissue is minimized by using the cutting current waveform.
Pure coagulating current delivers intermittent (low frequency) bursts of electrons under high voltage (force or pressure driving the current). The electrode is applied to the target tissue and the coagulating current denatures (alters the structure by heating) and dehydrates (removes water from) the tissue to produce hemostasis and charring. The tissue that is being coagulated is heated significantly in order to produce these effects, so that the coagulating current waveform carries a (much) higher risk of lateral thermal damage (burn injury) to surrounding (nontarget) tissue.
Many of the available electrical generators allow the surgeon to chose blends of these two (cutting and coagulating) waveforms, which vary in terms of the percentage of time that the current is on (flowing). This flexibility can be useful. In my own practice I often use blend #1, which provides a little bit of coagulation effect but predominantly delivers a cutting effect.
|

|