|
Controlled Ovarian Hyperstimulation: Pergonal #4
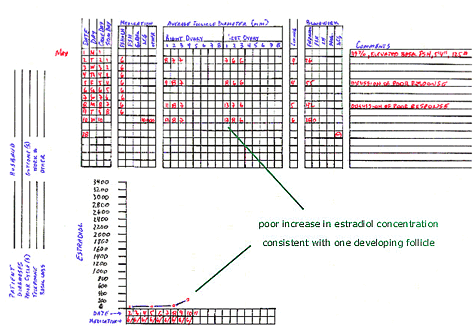
This (non-successful) cycle of controlled ovarian hyperstimulation (COH) with intrauterine insemination (IUI) illustrates
progress that may occur during COH cycles when there is very poor progress in either (or both) the follicular development or (and)
estradiol concentrations. Comments about this particular cycle might include:
1. This woman is 39 years old, which is an age that is often associated with a decreased ovarian reserve. Basal FSH concentrations were performed in an effort to assess ovarian reserve and indeed reflected a significant decrease (with intermittently elevated FSH concentrations). The decision whether to offer COH/IUI or IVF to patients in this situation is a difficult one since the literature suggests a poor response to the stimulation medication (menotropins) and a decreased reproductive potential for those eggs if they undergo IVF (a nonphysiologic environment for eggs in which they are removed from the body, fertilized in the laboratory, and incubated for several more days (in the laboratory) prior to being returned to the uterine cavity... sort of a stress test for eggs). In this case, the woman had the resources and desire to try a cycle of COH/IUI in order to give her a possible advantage over a natural cycle attempt at conception.
2. The highest dose of menotropins that I generally use in COH cycles (without a GnRH agonist) is 6 ampules per day. I have not found that 8 or 10 ampules a day improves the ovarian stimulation response, except possibly if a recombinant form of FSH (gonal F or follistim) is used. The recombinant forms of FSH seem to have a bit less of an effect on egg development when compared to the other menotropin medication available (note: drug representatives selling these agents do not really seem to think that this is true). Therefore, I generally add 1-2 ampules per dose to my usual amount of menotropin when using recombinant forms of FSH.
3. After 3 days of stimulation using 6 ampules (pergonal) a day the follicle development was poor and the rise in estradiol concentration was less than generally seen. Three more days of stimulation was suggested, to determine whether any effect could be seen
4. After 6 days of stimulation with 6 ampules (pergonal) a day there was a lead follicle measuring 13mm and the estradiol concentration increased to 132 pg/mL. Although not much of a response, the decision was to complete the cycle with a few more days of stimulation medication
5. After 8 days of stimulation, the lead follicle was 17mm and there was another smaller (12mm) follicle seen. In this case, one could reasonably stimulate the ovaries for an additional day or trigger ovulation with hCG. During IVF cycles, a mature egg is generally retrieved from all follicles that are 14mm or greater at the time of hCG, so I often use 14mm as the minimal follicular diameter reflecting egg maturation. Since the follicles were growing slowly in this case, I thought that it would probably take several days for the 12mm follicle to become 14mm (at which time the 17mm follicle would possibly be postmature) so I decided to trigger ovulation with hCG. In (other) cycles where there are multiple follicles that might mature with minimal additional stimulation, there is more of an incentive to continue to stimulate the ovaries.
6. Unfortunately, this cycle did not result in a pregnancy. The woman was advised that the menotropins did not seem to significantly enhance her reproductive potential, since she is ovulatory (makes one good egg per month spontaneously) and only made one mature egg with menotropins (involving daily injections, frequent monitoring with ultrasounds and bloodwork, considerable expense).
Additional Case Studies: COH Cycle 1 | COH Cycle 2
| COH Cycle 3
| COH Cycle 4 | COH Cycle 5
|

|