|
Controlled Ovarian Hyperstimulation: Pergonal #1
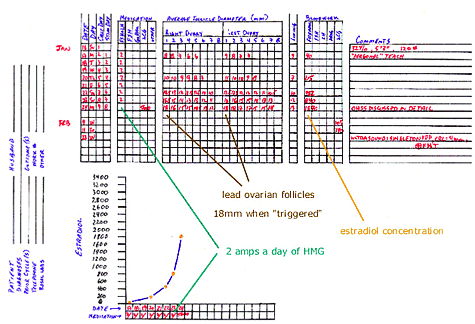
This (successful) cycle of controlled ovarian hyperstimulation (COH) with intrauterine insemination (IUI) illustrates the
progress that often occurs during COH cycles. Comments about this cycle might include:
1. The patient was 32 years old. A womans age is (roughly) related to her ovarian reserve and the number of ovarian follicles that
can be recruited to mature during any given month of COH. Although there is considerable individual variability in terms of the ovarian
response to menotropins, women generally respond less well after about the age of 35 and this decline in response is usually more
pronounced after the age of 40. Basal (cycle day 2-4) FSH concentration has been used extensively as an indicator of ovarian reserve,
and other tests have also been proposed (more recently) to assess this important variable. Basal estradiol, basal inhibin B
concentration, and the clomiphene citrate challenge test have been suggested to assess ovarian reserve. In my own practice, I
strongly recommend at least a basal FSH and estradiol concentration prior to a cycle of menotropin COH.
2. Prior to initiating a course of COH/IUI, I usually suggest a pelvic evaluation (laparoscopy and hysteroscopy) if not done
previously. The purpose of these procedures is to identify and treat any pelvic pathology that might interfere with reproductive
success. These same day (minor) surgical procedures allow the reproductive endocrinologist to identify and effectively treat important
factors like endometrial polyps, endometriosis or pelvic adhesions. Hysterosalpingography (or sonohysterography) has a high rate of
false negative results (reproductive endocrinologists find subtle lesions in the uterine cavity at the time of hysteroscopy about 30%
of the time after a hysterosalpingogram has been read as normal). Pelvic adhesions and endometriosis are usually only identifiable by
direct visualization (laparoscopy or open surgery), are often found in infertile women with no pain or other symptoms, and are not
seen with ultrasound or hysterosalpingography. Therefore, cleaning up the pelvis with a pelvic evaluation prior to initiating
treatment cycles of COH/IUI may significantly improve the womans reproductive potential (in many cases may allow the couple to
conceive without COH/IUI) or may optimize the success of the COH/IUI cycles (if required).
3. A normal (standard) dose of menotropins is 2 ampules a day when a GnRH agonist (such as lupron) is not required. This patient is
young and has an ideal body weight, so 2 ampules a day were initiated.
4. After 3 days of stimulation medication, the estradiol concentration is usually about 100-200 pg/mL. In this case the estradiol
concentration was 215 pg/mL. The follicular diameters are often about 10-11 mm after 3 days of menotropins (if not suppressed by a GnRH
agonist), which is what was found in this case. The dose of menotropins was therefore not reduced.
5. The estradiol concentration often doubles between stimulation day 4 and 6, and in this case the estradiol concentration rose by
slightly greater than 2 fold. The follicular diameter often increases by 1-2 mm a day during menotropin stimulation, and this was
found to be the case during this patients cycle. The menotropin dose was not decreased at this point.
6. The estradiol concentration often increases about 2-3 fold every other day during the middle of a COH (menotropin) stimulation
cycle (without GnRH agonist). From stimulation day 7 to stimulation day 8 the estradiol concentration rose by greater than 50%
(482 pg/mL to 840 pg/mL), and at this point the menotropin dosage might have been decreased. However, the estradiol concentration
of 840 pg/mL was not worrisome, the increase in ovarian follicular diameters was healthy, and it was thought that only one more day
of stimulation would be required. Therefore, the menotropin dose was not decreased.
7. The estradiol concentration often increases by about 2 fold on the last day of stimulation using menotropins without GnRH agonist
(it doubles up). In this situation, the estradiol concentration rose from 840 pg/mL to 1840 pg/mL and the leading (average)
follicular diameters were 18 mm. I most often trigger ovulation when the lead follicle is 18mm.
8. COH/IUI cycles without GnRH agonists often involve 5-7 days of menotropin stimulation.
9. The initial hCG titer was 105 IU/L, which is ideal for two weeks after ovulation (ovulation generally occurs about 36 hours
after hCG trigger of ovulation). The rate of rise of hCG was normal and an ultrasound revealed a normal singleton intrauterine
pregnancy 4 weeks after ovulation (6 weeks gestation). I usually find an embryo that has a crown to rump length (CRL) of about
4 mm with an active fetal heart beat (FHT) at 6 weeks gestational age (4 weeks from ovulation).
Additional Case Studies: COH Cycle 1 | COH Cycle 2
| COH Cycle 3
| COH Cycle 4 | COH Cycle 5
|

|